Let’s play detective for a moment. What if I told you that your gums could provide clues about your overall health? In many cases, gum disease isn’t just a dental woe. It can be an early alert system, pointing towards more systemic issues like diabetes.
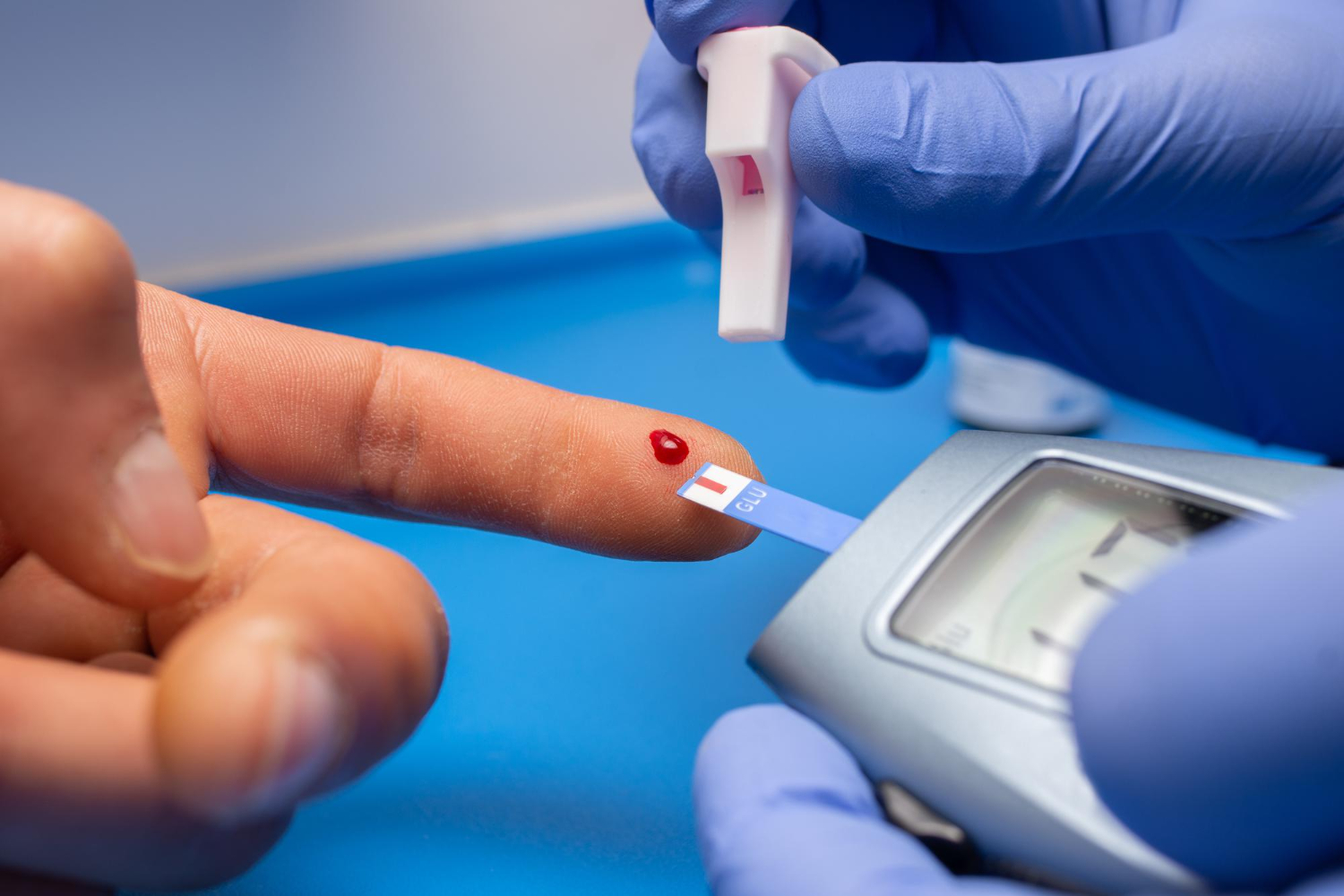
How Gum Disease Can Signal Diabetes: Long before a formal diabetes diagnosis, gum disease might rear its head. It’s not uncommon for dentists to identify signs of diabetes in patients who came in for what they thought was just a “routine” dental issue. Elevated blood sugar levels can compromise the immune system, making it harder to fend off oral infections. If you’re consistently battling gum issues, it might be time to peek at your blood sugar numbers.
Inflammation: The Common Culprit: Inflammation is like the body’s alarm system. And both diabetes and gum disease share this red flag. Elevated blood sugar levels can cause inflammation throughout the body, including the gums. Similarly, gum disease in its more severe forms (like periodontitis) can lead to widespread inflammation. This shared inflammatory response links diabetes and gum disease in a close dance.
The Vicious Cycle: Severe gum disease doesn’t just stop at affecting your mouth. It can also exacerbate diabetes. As the body fights the gum infection, blood sugar levels can spike. For diabetics, this makes blood sugar management even trickier, creating a feedback loop that’s hard to break.
Beyond the Gums: Other Dental Concerns for Diabetics
Gum disease might be the headline act, but there’s a supporting cast of dental concerns that diabetics should be aware of.
Delayed Healing: Ever noticed that a minor mouth injury, like a bite on the inner cheek or tongue, takes longer to heal if you have diabetes? Elevated blood sugar levels can impair blood flow, delaying the healing process. This is especially pertinent after dental procedures.
The Fungus Among Us: Diabetics are more susceptible to oral fungal infections like thrush. A combination of reduced salivary flow and increased sugar in saliva can be an open invitation for candida, the fungus responsible for thrush, to flourish.
The Unsavory Link to Bad Breath: Persistent bad breath or a bad taste in the mouth, despite your best oral hygiene practices, could be linked to diabetes. It’s all tied to how the body sometimes breaks down fats instead of sugars, leading to the release of ketones, which have a distinct foul odor.
Dr. Dawson often says, “Your mouth is a window to your overall health.” And for diabetics, this rings truer than ever. By keeping a vigilant eye on oral health and understanding the deeper connections, you can better navigate the challenges diabetes presents.
Gum Disease: A Signal and Contributor
When most of us think about gum disease, we imagine it as a dental problem, isolated from the rest of our body. However, if the gums could talk, they might just spill the beans on other underlying health conditions, especially diabetes.
Spotting the Early Signs: Sometimes, your body drops hints in unexpected ways. Persistent gum problems, such as bleeding or inflammation, might not just be about neglecting to floss. They could be early indicators of diabetes. This is because high blood sugar can weaken our body’s capacity to fight bacteria, making the gums more vulnerable.
The Inflammation Connection: Think of inflammation as the body’s smoke alarm. Both diabetes and gum disease send out this signal loud and clear. High blood sugar levels can lead to inflammation throughout the body. At the same time, gum disease, particularly periodontitis, is an inflammatory condition affecting the tissues surrounding teeth. When both conditions co-exist, they can amplify each other.
Feedback Loop Frenzy: It gets more intriguing. Severe gum disease can be more than just a symptom of diabetes; it can also be a contributor. Infections in the gums can lead to an increased resistance to insulin, making blood sugar control even more challenging. It’s a two-way street of influence and effect.
Beyond the Gums: Other Dental Concerns for Diabetics
But the story doesn’t end with the gums. Diabetes casts a wider net, influencing various aspects of oral health.
The Slow Road to Recovery: Diabetes can play spoilsport with the body’s natural healing process. So, whether it’s recovering from a dental extraction or just a pesky mouth ulcer, healing might take longer than usual for those with diabetes.
Oral Fungal Fest: A drier mouth and higher sugar levels in the saliva create a perfect storm for fungal infections. Oral thrush, characterized by white patches and soreness in the mouth, is more common among diabetics.
Bad Breath and Diabetes: Ever experienced stubborn bad breath that refuses to budge? If you’re a diabetic, this might be due to high levels of ketones in your blood, a by-product of your body burning fat instead of glucose for energy. It’s more than just an oral hygiene issue; it’s a sign that your diabetes isn’t under optimal control.
The lesson here is clear: for those with diabetes, a regular dental check-up isn’t just about cavities or cleanings; it’s a crucial part of overall health management. Dr. Turke often reminds his patients, “The mouth is a mirror to the body.” And indeed, when it comes to diabetes, this reflection offers deep insights.
Proactive Steps for Diabetics: Ensuring Oral Health
Navigating life with diabetes requires awareness, proactive measures, and a sprinkle of diligence. When it comes to ensuring optimal oral health for diabetics, a few tailored steps can make all the difference.
Routine Dental Visits: Not Just a Check-up, It’s a Check-In: Regular dental appointments go beyond just a quick look at your teeth. They are opportunities to catch early signs of potential issues, get professional cleanings to reduce the risk of gum diseases, and discuss any concerns directly with experts. For diabetics, these visits can be instrumental in preventing complications and staying ahead of potential problems.
Tailored Oral Hygiene for Diabetics: Everyone should brush and floss daily, but if you have diabetes, there are some additional measures to consider. Using a specialized toothpaste designed for gum health, ensuring you clean your tongue to combat bad breath, and possibly even adopting an anti-fungal mouthwash can be beneficial. And let’s not forget about staying hydrated to combat dry mouth!
Controlled Blood Sugar, Healthier Mouth: The relationship is direct and undeniable. When you keep your blood sugar levels in check, you reduce the risks associated with gum diseases and other oral health complications. It’s a symbiotic relationship: a healthier mouth can assist in better diabetes management, and controlled diabetes ensures a happier, healthier mouth.
Smile Science Dental Spa: Your Partner in Managing Diabetes and Oral Health
Living with diabetes doesn’t mean walking the path alone. At Smile Science Dental Spa, we’re committed to partnering with you, ensuring your oral health complements your diabetes management plan.
Expertise with a Personal Touch: Drs. Dawson and Turke aren’t just equipped with the latest knowledge on diabetes and oral health; they bring a personal touch to every consultation. Understanding the unique challenges faced by diabetic patients, they tailor dental care recommendations that align with your overall health objectives.
A Comprehensive Approach: At Smile Science, we believe in a holistic approach. Whether it’s suggesting the best oral hygiene products for diabetics, providing dietary advice to counteract dry mouth, or coordinating with your primary care physician, our focus is comprehensive care. It’s not just about reacting to issues but proactively preventing them.
Remember, your journey with diabetes is intertwined with your oral health, and at Smile Science Dental Spa, we’re dedicated to ensuring that connection remains a healthy, positive one.
The Broader Picture: Overall Health and Wellness
We often draw boundaries between different aspects of our health, but in reality, everything is connected in a beautiful, intricate dance. Just as the eyes are said to be a window to the soul, your mouth can be a window to your general well-being.
Oral Health: Not an Island: It’s a misconception to think of oral health as limited to teeth and gums. Problems in the mouth can be symptoms of issues elsewhere. Think of your body as a well-tuned orchestra, and your mouth, the lead violinist. When the violinist falters, the entire symphony feels the discord.
Diet, Check-ups, and the Big Picture: You are what you eat, and so is your mouth. A balanced diet not only fuels your body but ensures your teeth and gums get the nutrients they need. Meanwhile, regular medical check-ups, much like your routine dental visits, ensure all systems are working in harmony. It’s about catching potential issues before they crescendo into significant problems.
Conclusion: Empowerment Through Knowledge and Care
Knowledge isn’t just power; it’s empowerment. As we’ve journeyed through the interplay of diabetes, oral health, and overall wellness, it’s clear that understanding is our most potent weapon.
Awareness and Proaction: Recognizing signs, staying ahead of potential problems, and adopting proactive measures can significantly influence the trajectory of your health journey. But this isn’t a solo act. It’s a partnership between you and your healthcare providers.
Smile Science Dental Spa’s Pledge: At the heart of our practice lies a deep-seated commitment to every patient’s well-being. Dr. Dawson, Dr. Turke, and the entire team are here not just as dental professionals but as partners in your broader health journey. Every check-up, consultation, or procedure is a step towards a healthier you, both inside and out.
Remember, your smile isn’t just about aesthetics; it’s a reflection of your holistic health. And at Smile Science Dental Spa, we’re dedicated to ensuring every smile radiates wellness and confidence.
Further Reading
- Oral Health and Type 2 Diabetes
- Diabetes and Oral Health: A Case-control Study
- Oral Health Messiers: Diabetes Mellitus Relevance
- State of Evidence on Oral Health Problems in Diabetic Patients: A Critical Review of the Literature
- The burden of Diabetes, Its Oral Complications and Their Prevention and Management